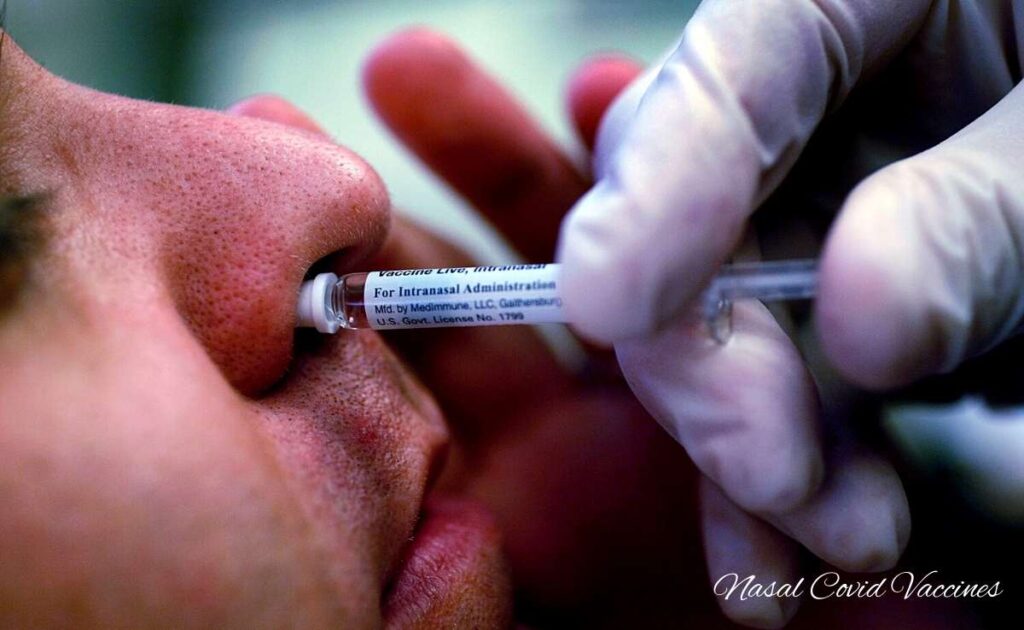
India is preparing the first intranasal preventative drug for the Covid outbreak, and scientists are optimistic about the potential of mucosal immunizations to avert even minor cases of the disease and slow its spread.
Mucosal vaccines, which are designed to protect the lining of the mouth and throat, may one day be able to prevent the spread of even relatively harmless diseases.
Vaccines that target the mucosal layer of the mouth and throat may be able to prevent even minor illnesses from spreading.
Nasal, non-invasive, and less expensive alternatives to injectable vaccines are being studied by scientists as a possible solution to the world’s ever-changing Covid wave, which presents new hurdles at every turn due to the constant emergence of new strains.
What Is Nasal COVID Vaccine
The first intranasal COVID-19 vaccine, iNCOVACC (BBV154), was developed by Bharat Biotech and approved for emergency use only by the Drugs Controller General of India earlier this month. This go-ahead is strictly for people who live in India. Vaccine availability to the general public is currently undetermined.
A single dose of the COVID-19 vaccine created by Pfizer or AstraZeneca lowered the risk of spreading SARS-CoV-2 to close contacts by as much as 50%, according to a trial involving over 365,000 homes in the United Kingdom.
This result was reached after an extensive study of the vaccine’s effectiveness. Research in the UK is the source of these numbers.
Although vaccines have been found to reduce the severity of sickness and symptoms produced by COVID-19, their ability to halt the transmission of the coronavirus is still up for debate.
Public Health England researchers Kevin Dunbar, Gavin Cabrera, and others in London looked for cases of SARS-CoV-2 infection in persons who had received either vaccine. They next determined the rate at which those individuals were infecting their immediate family members.
Those who had been inoculated for at least 21 days were nonetheless at risk of having a positive test result for the virus, according to the study’s authors.
Even while the rate of transmission is reduced by 40-50% compared to households where the first positive test result was not due to vaccination, the virus is still disseminated in these homes.
The statistical study supported the existence of a huge gap. All things considered, the outcomes of both immunizations were similar. Since the findings haven’t been peer-reviewed, we can’t make any definitive claims regarding them just yet.
The COVID-19 outbreak in Santiago, Chile, had the greatest impact on the city’s most disadvantaged citizens. Overcrowding, a lack of quick access to healthcare, and the difficulties of working from home were all factors that contributed to this problem.
This took place as a consequence of the simultaneous occurrence of several separate events.
According to research conducted by Gonzalo Mena and his colleagues at the Harvard T.H. Chan School of Public Health in Boston, Massachusetts, death rates were discovered to be significantly higher in low-income regions of Santiago. This was particularly the case among individuals under the age of 80.
The findings of the studies carried out in Chile came to the same conclusion.
The findings of this investigation were subsequently presented in the highly regarded publication Science, which is a scientific journal.
To explain the disparity, the researchers came up with several different possibilities. In contrast to regions with higher incomes, places with lower incomes were shown to have higher rates of SARS-CoV-2-positive individuals.
This was the case due to the higher prevalence of poverty in those places. It is reasonable to presume that this indicates that insufficient testing was conducted in the region, which prevented efficient case-based prioritizing of resources to fight the pandemic.
This is a result of insufficient testing being conducted in the region. There was just a quarter of the number of hospital beds available per 10,000 inhabitants in regions that had lower earnings than there were in regions that had greater earnings.
In neighborhoods with low incomes, ninety percent of COVID-19-related deaths that occurred outside of hospitals and other healthcare organizations were recorded.
While just 55% of COVID-19 deaths could be attributed to healthcare facilities located in a more affluent part of the city. Only 55% of COVID-19 deaths could be traced back to medical institutions in this more affluent part of the city.
Conclusion
The authors of the study discovered that people in low-income neighborhoods were more active at times of the day when they should have been at home. The researchers were able to get to this conclusion by incorporating data on cell phone locations into their investigation.
This is most likely attributable to the fact that a greater proportion of the local people held jobs that required them to be absent from their homes for extended periods.
Also, Read More About – Zerodol Sp Tablet: Uses, Side Effects, Composition, Price & Dosage?
Chocolate & Gummies: Shroom Edibles For A Better Psychedelic Experience